After reading Chapter 9 and reviewing the lecture power point (located in lectures tab), please answer the following questions.
1. Describe the link between quality and safety in the healthcare setting.
2. Discuss the role of the nurse in quality improvement.
3. Describe nursing-sensitive measurements and why they are important in Nursing care delivery.
2
The Pedagogy Role Development in
Professional Nursing Practice, Fourth Edition
drives comprehension through various
strategies that meet the learning needs of
students, while also generating enthusiasm
about the topic. This interactive approach
addresses different learning styles, making
this the ideal text to ensure mastery of key
concepts. The pedagogical aids that appear in
most chapters include the following:
3
4
5
6
World Headquarters
Jones & Bartlett Learning
5 Wall Street
Burlington, MA 01803
978-443-5000
info@jblearning.com
www.jblearning.com
Jones & Bartlett Learning books and products are available through most bookstores and online
booksellers. To contact Jones & Bartlett Learning directly, call 800-832-0034, fax 978-443-8000,
or visit our website, www.jblearning.com.
Substantial discounts on bulk quantities of Jones & Bartlett Learning publications are available
to corporations, professional associations, and other qualified organizations. For details and
specific discount information, contact the special sales department at Jones & Bartlett Learning
via the above contact information or send an email to specialsales@jblearning.com.
Copyright © 2017 by Jones & Bartlett Learning, LLC, an Ascend Learning Company All rights
reserved. No part of the material protected by this copyright may be reproduced or utilized in any
form, electronic or mechanical, including photocopying, recording, or by any information storage
and retrieval system, without written permission from the copyright owner.
The content, statements, views, and opinions herein are the sole expression of the respective
authors and not that of Jones & Bartlett Learning, LLC. Reference herein to any specific
commercial product, process, or service by trade name, trademark, manufacturer, or otherwise
does not constitute or imply its endorsement or recommendation by Jones & Bartlett Learning,
LLC and such reference shall not be used for advertising or product endorsement purposes. All
trademarks displayed are the trademarks of the parties noted herein. Role Development in
Professional Nursing Practice, Fourth Edition is an independent publication and has not been
authorized, sponsored, or otherwise approved by the owners of the trademarks or service marks
referenced in this product.
There may be images in this book that feature models; these models do not necessarily endorse,
represent, or participate in the activities represented in the images. Any screenshots in this product
are for educational and instructive purposes only. Any individuals and scenarios featured in the
case studies throughout this product may be real or fictitious, but are used for instructional
purposes only.
The authors, editor, and publisher have made every effort to provide accurate information.
However, they are not responsible for errors, omissions, or for any outcomes related to the use of
the contents of this book and take no responsibility for the use of the products and procedures
described. Treatments and side effects described in this book may not be applicable to all people;
likewise, some people may require a dose or experience a side effect that is not described herein.
Drugs and medical devices are discussed that may have limited availability controlled by the Food
and Drug Administration (FDA) for use only in a research study or clinical trial. Research, clinical
practice, and government regulations often change the accepted standard in this field. When
consideration is being given to use of any drug in the clinical setting, the health care provider or
reader is responsible for determining FDA status of the drug, reading the package insert, and
reviewing prescribing information for the most up-to-date recommendations on dose, precautions,
and contraindications, and determining the appropriate usage for the product. This is especially
important in the case of drugs that are new or seldom used.
08323-1
7
Production Credits
VP, Executive Publisher: David D. Cella Executive Editor: Amanda Martin Acquisitions Editor:
Teresa Reilly Editorial Assistant: Danielle Bessette Production Editor: Vanessa Richards Senior
Marketing Manager: Jennifer Scherzay VP, Manufacturing and Inventory Control: Therese Connell
Composition: Integra Software Services Pvt. Ltd.
Cover Design: Kristin E. Parker Rights & Media Specialist: Wes DeShano Media Development
Editor: Shannon Sheehan Cover Image: © robertiez/iStock/Getty Images Plus/Getty Printing and
Binding: RR Donnelley Cover Printing: RR Donnelley
Library of Congress Cataloging-in-Publication Data Role development in professional nursing
practice / [edited by] Kathleen Masters. – Fourth edition.
p. ; cm.
Includes bibliographical references and index.
ISBN 978-1-284-07832-9 (pbk.) I. Masters, Kathleen, editor.
[DNLM: 1. Nursing–standards. 2. Nursing–trends. 3. Nurse’s Role. 4. Philosophy, Nursing. 5.
Professional Practice. WY 16]
RT82
610.73–dc23
2015022040
6048
Printed in the United States of America 19 18 17 16 15 10 9 8 7 6 5 4 3 2 1
8
Dedication
This book is dedicated to my Heavenly Father
and to my loving family: my husband, Eddie,
and my two daughters, Rebecca and Rachel.
Words cannot express my appreciation for their
ongoing encouragement and support throughout
my career.
9
CONTENTS
Preface
Contributors
UNIT I: FOUNDATIONS OF PROFESSIONAL NURSING PRACTICE
1
A History of Health Care and Nursing
Karen Saucier Lundy and Kathleen Masters
Classical Era
Middle Ages
The Renaissance
The Dark Period of Nursing
The Industrial Revolution
And Then There Was Nightingale…
Continued Development of Professional Nursing in the United Kingdom
The Development of Professional Nursing in Canada
The Development of Professional Nursing in Australia
Early Nursing Education and Organization in the United States
The Evolution of Nursing in the United States: The First Century of Professional
Nursing
The New Century
International Council of Nurses
Conclusion
References
2
Frameworks for Professional Nursing Practice
Kathleen Masters
10
Overview of Selected Nursing Theories
Nurse of the Future: Nursing Core Competencies
Overview of Selected Non-Nursing Theories
Relationship of Theory to Professional Nursing Practice
Conclusion
References
3
Philosophy of Nursing
Mary W. Stewart
Philosophy
Early Philosophy
Paradigms
Beliefs
Values
Developing a Personal Philosophy of Nursing
Conclusion
References
4
Foundations of Ethical Nursing Practice
Janie B. Butts and Karen L. Rich
Ethics
Ethical Theories and Approaches
Professional Ethics and Codes
Ethical Analysis and Decision Making in Nursing
Conclusion
References
5
Social Context of Professional Nursing
Mary W. Stewart, Katherine Elizabeth Nugent, Rowena W. Elliott, and
11
Kathleen Masters
Nursing’s Social Contract with Society
Public Image of Nursing
The Gender Gap
Changing Demographics and Cultural Competence
Access to Health Care
Societal Trends
Trends in Nursing
Conclusion
References
6
Education and Socialization to the Professional Nursing Role
Kathleen Masters and Melanie Gilmore
Professional Nursing Roles and Values
The Socialization (or Formation) Process
Facilitating the Transition to Professional Practice
Conclusion
References
7
Advancing and Managing Your Professional Nursing Career
Mary Louise Coyne and Cynthia Chatham
Nursing: A Job or a Career?
Trends That Impact Nursing Career Decisions
Showcasing Your Professional Self
Mentoring
Education and Lifelong Learning
Professional Engagement
Expectations for Your Performance
12
Taking Care of Self
Conclusion
References
UNIT II: PROFESSIONAL NURSING PRACTICE AND THE MANAGEMENT OF
PATIENT CARE
8
Patient Safety and Professional Nursing Practice
Jill Rushing and Kathleen Masters
Patient Safety
Critical Thinking, Clinical Judgment, and Clinical Reasoning in Nursing Practice
Conclusion
References
9
Quality Improvement and Professional Nursing Practice
Kathleen Masters
Healthcare Quality
Measurement of Quality
The Role of the Nurse in Quality Improvement
Conclusion
References
Professional Nursing Practice
10 Evidence-Based
Kathleen Masters
Evidence-Based Practice: What Is It?
Barriers to Evidence-Based Practice
Promoting Evidence-Based Practice
Searching for Evidence
Evaluating the Evidence
Implementation Models for Evidence-Based Practice
13
Conclusion
References
11
Patient-Centered Care and Professional Nursing Practice
Kathleen Masters
Dimensions of Patient-Centered Care
Communication as a Strategy to Support Patient-Centered Care
Patient Education as a Strategy to Support Patient-Centered Care
Evaluation of Patient-Centered Care
Conclusion
References
in Professional Nursing Practice
12 Informatics
Kathleen Masters and Cathy K. Hughes
Informatics: What Is It?
The Impact of Legislation on Health Informatics
Nursing Informatics Competencies
Basic Computer Competencies
Information Literacy
Information Management
Current and Future Trends
Conclusion
References
and Collaboration in Professional Nursing Practice
13 Teamwork
Sharon Vincent and Kathleen Masters
Healthcare Delivery System
Nursing Models of Patient Care
Roles of the Professional Nurse
14
Interprofessional Teams and Healthcare Quality and Safety
Interprofessional Collaborative Practice Domains
Interprofessional Team Performance and Communication
Conclusion
References
Issues in Professional Nursing Practice
14 Ethical
Janie B. Butts and Karen L. Rich
Relationships in Professional Practice
Moral Rights and Autonomy
Social Justice
Death and End-of-Life Care
Conclusion
References
and the Professional Nurse
15 Law
Kathleen Driscoll, Kathleen Masters, and Evadna Lyons
The Sources of Law
Classification and Enforcement of the Law
Nursing Scope and Standards
Malpractice and Negligence
Nursing Licensure
Professional Accountability
Conclusion
References
Appendix A Standards of Professional Nursing Practice
Appendix B Provisions of Code of Ethics for Nurses
Appendix C The ICN Code of Ethics for Nurses
15
Glossary
Index
16
PREFACE
Although the process of professional development is a lifelong journey, it is a
journey that begins in earnest during the time of initial academic preparation.
The goal of this book is to provide nursing students with a road map to help
guide them along their journey as a professional nurse.
This book is organized into two units. The chapters in the first unit focus
on the foundational concepts that are essential to the development of the
individual professional nurse. The chapters in Unit II address issues related to
professional nursing practice and the management of patient care, specifically
in the context of quality and safety. In the fourth edition, the chapter content
is conceptualized, when applicable, around nursing competencies,
professional standards, and recommendations from national groups, such as
Institute of Medicine reports.
The chapters included in Unit I provide the student nurse with a basic
foundation in areas such as nursing history, theory, philosophy, ethics,
socialization into the nursing role, and the social context of nursing. All
chapters have been updated, and several chapters in Unit I have been
expanded in this edition. Revisions to the chapter on nursing history include
the addition of contributions of prominent nurses and achievements related
to nursing in the United Kingdom, Canada, and Australia. The theory
chapter now includes additional nursing theorists as well as a brief overview
of several non-nursing theories frequently used in nursing research and
practice. The social context of nursing chapter now incorporates not only
societal trends, but also trends in nursing practice and education. The
chapter related to professional career development in nursing has been
completely rewritten for this edition.
The chapters in Unit II are more directly related to patient care
management. In the fourth edition, Unit II chapter topics are presented in the
context of quality and safety. Chapter topics include the role of the nurse in
patient safety, the role of the nurse in quality improvement, evidence-based
nursing practice, the role of the nurse in patient-centered care, informatics in
nursing practice, the role of the nurse related to teamwork and collaboration,
ethical issues in nursing practice, and the law as it relates to patient care and
nursing. Most Unit II chapters have undergone major revisions with a refocus
of the content on recommended nursing and healthcare competencies.
The fourth edition continues to incorporate the Nurse of the Future:
Nursing Core Competencies throughout each chapter. The Nurse of the
Future: Nursing Core Competencies “emanate from the foundation of
nursing knowledge” (Massachusetts Department of Higher Education, 2010,
17
p. 4) and are based on the American Association of Colleges of Nursing’s
Essentials of Baccalaureate Education for Professional Nursing Practice,
National League for Nursing Council of Associate Degree Nursing
competencies, Institute of Medicine recommendations, Quality and Safety
Education for Nurses (QSEN) competencies, and American Nurses
Association standards, as well as other professional organization standards
and recommendations. The 10 competencies included in the model are
patient-centered care, professionalism, informatics and technology, evidencebased practice, leadership, systems-based practice, safety, communication,
teamwork and collaboration, and quality improvement. Essential knowledge,
skills, and attitudes (KSA) reflecting cognitive, psychomotor, and affective
learning domains are specified for each competency. The KSA identified in
the model reflect the expectations for initial nursing practice following the
completion of a prelicensure professional nursing education program
(Massachusetts Department of Higher Education, 2010, p. 4).
18
Source: Modified from Massachusetts Department of Higher Education. (2010). Nurse of the
future: Nursing core competencies (p. 5). Retrieved from
http://www.mass.edu/currentinit/documents/NursingCoreCompetencies.pdf
The Nurse of the Future: Nursing Core Competencies graphic illustrates
through the use of broken lines the reciprocal and continuous relationship
between each of the competencies and nursing knowledge, that the
competencies can overlap and are not mutually exclusive, and that all
competencies are of equal importance. In addition, nursing knowledge is
placed as the core in the graphic to illustrate that nursing knowledge reflects
the overarching art and science of professional nursing practice
(Massachusetts Department of Higher Education, 2010, p. 4).
This new edition has competency boxes throughout the chapters that link
examples of the KSA appropriate to the chapter content to Nurse of the
Future: Nursing Core Competencies required of entry-level professional
19
nurses. The competency model in its entirety is available online at
www.mass.edu/currentinit/documents/NursingCoreCompetencies.pdf.
This new edition continues to use case studies, congruent with Benner,
Sutphen, Leonard, and Day’s (2010) Carnegie Report recommendations that
nursing educators teach for “situated cognition” using narrative strategies to
lead to “situated action,” thus increasing the clinical connection in our
teaching or that we teach for “clinical salience.” In addition, critical thinking
questions are included throughout each chapter to promote student reflection
on the chapter concepts. Classroom activities are also provided based on
chapter content. Additional resources not connected to this text, but
applicable to the content herein, include a toolkit focused on the nursing core
competencies
available
at
www.mass.edu/nahi/documents/ToolkitFirst%20Edition-May%202014-r1.pdf and teaching activities related to
nursing
competencies
available
on
the
QSEN
website
at
www.qsen.org/teaching-strategies/.
Although the topics included in this textbook are not inclusive of all that
could be discussed in relationship to the broad theme of role development in
professional nursing practice, it is my prayer that the subjects herein make a
contribution to the profession of nursing by providing the student with a
solid foundation and a desire to grow as a professional nurse throughout the
journey that we call a professional nursing career. Let the journey begin.
—Kathleen Masters
References
Benner, P., Sutphen, M., Leonard, V., & Day, L. (2010). Educating nurses: A call for radical
transformation. San Francisco, CA: Jossey-Bass.
Massachusetts Department of Higher Education. (2010). Nurse of the future: Nursing core
competencies.
Retrieved
from
http://www.mass.edu/currentinit/documents/NursingCoreCompetencies.pdf
20
CONTRIBUTORS
Janie B. Butts, PhD, RN
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Cynthia Chatham, DSN, RN
University of Southern Mississippi College of Nursing
Long Beach, Mississippi
Mary Louise Coyne, DNSc, RN
University of Southern Mississippi College of Nursing
Long Beach, Mississippi
Kathleen Driscoll, JD, MS, RN
University of Cincinnati College of Nursing
Cincinnati, Ohio
Rowena W. Elliott, PhD, RN, FAAN
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Melanie Gilmore, PhD, RN
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Cathy K. Hughes, DNP, RN
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Karen Saucier Lundy, PhD, RN, FAAN
Professor Emeritus
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Evadna Lyons, PhD, RN
East Central Community College School of Nursing
Decatur, Mississippi
Katherine Elizabeth Nugent, PhD, RN
Dean, College of Nursing University of Southern Mississippi Hattiesburg,
Mississippi Karen L. Rich, PhD, RN
University of Southern Mississippi College of Nursing
Long Beach, Mississippi
21
Jill Rushing, MSN, RN
University of Southern Mississippi College of Nursing
Hattiesburg, Mississippi Mary W. Stewart, PhD, RN
Director of PhD Program
University of Mississippi Medical Center School of Nursing
Jackson, Mississippi
Sharon Vincent, DNP, RN, CNOR
University of North Carolina College of Nursing
Charlotte, North Carolina
22
UNIT I
Foundations of Professional Nursing Practice
23
CHAPTER 1
A History of Health Care and Nursing
Karen Saucier Lundy and Kathleen Masters
24
Learning Objectives
After completing this chapter, the student should be able to:
1. Identify social, political, and economic influences on the
development of professional nursing practice.
2. Identify important leaders and events that have significantly
affected the development of professional nursing practice.
25
Key Terms and Concepts
» Greek era
» Roman era
» Deaconesses
» Florence Nightingale
» Reformation
» Chadwick Report
» Shattuck Report
» William Rathbone
» Ethel Fenwick
» Jeanne Mance
» Mary Agnes Snively
» Goldmark Report
» Brown Report
» Isabel Hampton Robb
» American Nurses Association (ANA)
» Lavinia Lloyd Dock
» American Journal of Nursing (AJN)
» Margaret Sanger
» Lillian Wald
» Jane A. Delano
» Annie Goodrich
» Mary Brewster
» Henry Street Settlement
» Elizabeth Tyler
» Jessie Sleet Scales
» Dorothea Lynde Dix
» Clara Barton
26
» Frontier Nursing Service
» Mary Breckinridge
» Mary D. Osborne
» Frances Payne Bolton
» International Council of Nurses (ICN)
Although no specialized nurse role per se developed in early civilizations,
human cultures recognized the need for nursing care. The truly sick person
was weak and helpless and could not fulfill the duties that were normally
expected of a member of the community. In such cases, someone had to
watch over the patient, nurse him or her, and provide care. In most societies,
this nurse role was filled by a family member, usually female. As in most
cultures, the childbearing woman had special needs that often resulted in a
specialized role for the caregiver. Every society since the dawn of time had
someone to nurse and take care of the mother and infant around the
childbearing events. In whatever form the nurse took, the role was associated
with compassion, health promotion, and kindness (Bullough & Bullough,
1978).
27
Classical Era
More than 4,000 years ago, Egyptian physicians and nurses used an
abundant pharmacological repertoire to cure the ill and injured. The Ebers
Papyrus lists more than 700 remedies for ailments ranging from snakebites to
puerperal fever (Kalisch & Kalisch, 1986). Healing appeared in the Egyptian
culture as the successful result of a contest between invisible beings of good
and evil (Shryock, 1959). Around 1000 B.C., the Egyptians constructed
elaborate drainage systems, developed pharmaceutical herbs and
preparations, and embalmed the dead. The Hebrews formulated an elaborate
hygiene code that dealt with laws governing both personal and community
hygiene, such as contagion, disinfection, and sanitation through the
preparation of food and water. The Jewish contribution to health is greater
in sanitation than in their concept of disease. Garbage and excreta were
disposed of outside the city or camp, infectious diseases were quarantined,
spitting was outlawed as unhygienic, and bodily cleanliness became a
prerequisite for moral purity. Although many of the Hebrew ideas about
hygiene were Egyptian in origin, the Hebrews were the first to codify them
and link them with spiritual godliness (Bullough & Bullough, 1978).
Disease and disability in the Mesopotamian area were considered a great
curse, a divine punishment for grievous acts against the gods. Experiencing
illness as punishment for a sin linked the sick person to anything even
remotely deviant. Not only was the person suffering from the illness, but he
or she also was branded by all of society as having deserved it. Those who
obeyed God’s law lived in health and happiness, and those who transgressed
the law were punished with illness and suffering. The sick person then had to
make atonement for the sins, enlist a priest or other spiritual healer to lift the
curse, or live with the illness to its ultimate outcome (Bullough & Bullough,
1978). Nursing care by a family member or relative would be needed,
regardless of the outcome of the sin, curse, disease-atonement-recovery, or
death cycle. This logic became the basis for explanation of why some people
“get sick and some don’t” for many centuries and still persists to some
degree in most cultures today.
The Greeks and Health
In Greek mythology, the god of medicine, Asclepias, cured disease. One of
his daughters, Hygeia, from whom we derive the word hygiene, was the
goddess of preventive health and protected humans from disease. Panacea,
Asclepias’ other daughter, was known as the all-healing “universal remedy,”
and today her name is used to describe any ultimate cure-all in medicine. She
28
was known as the “light” of the day, and her name was invoked and shrines
built to her during times of epidemics (Brooke, 1997).
During the Greek era, Hippocrates of Cos emphasized the rational
treatment of sickness as a natural rather than god-inflicted phenomenon.
Hippocrates (460–370 B.C.) is considered the father of medicine because of
his arrangements of the oral and written remedies and diseases, which had
long been secrets held by priests and religious healers, into a textbook of
medicine that was used for centuries (Bullough & Bullough, 1978).
In Greek society, health was considered to result from a balance between
mind and body. Hippocrates wrote a most important book, Air, Water and
Places, which detailed the relationship between humans and the
environment. This is considered a milestone in the eventual development of
the science of epidemiology as the first such treatise on the connectedness of
the web of life. This topic of the relationship between humans and their
environment did not reoccur until the development of bacteriology in the late
1800s (Rosen, 1958).
Perhaps the idea that most damaged the practice and scientific theory of
medicine and health for centuries was the doctrine of the four humors, first
spoken of by Empedocles of Acragas (493–433 B.C.). Empedocles was a
philosopher and a physician, and as a result, he synthesized his cosmological
ideas with his medical theory. He believed that the same four elements that
made up the universe were found in humans and in all animate beings
(Bullough & Bullough, 1978). Empedocles believed that man was a
microcosm, a small world within the macrocosm, or external environment.
The four humors of the body (blood, bile, phlegm, and black bile)
corresponded to the four elements of the larger world (fire, air, water, and
earth) (Kalisch & Kalisch, 1986). Depending on the prevailing humor, a
person was sanguine, choleric, phlegmatic, or melancholic. Because of this
strongly held and persistent belief in the connection between the balance of
the four humors and health status, treatment was aimed at restoring the
appropriate balance of the four humors through the control of their
corresponding elements. Through manipulating the two sets of opposite
qualities—hot and cold, wet and dry—balance was the goal of the
intervention. Fire was hot and dry, air was hot and wet, water was cold and
wet, and earth was cold and dry. For example, if a person had a fever, cold
compresses would be prescribed; for a chill the person would be warmed.
Such doctrine gave rise to faulty and ineffective treatment of disease that
influenced medical education for many years (Taylor, 1922).
Plato, in The Republic, details the importance of recreation, a balanced
mind and body, nutrition, and exercise. A distinction was made among
gender, class, and health as early as the Greek era; only males of the
aristocracy could afford the luxury of maintaining a healthful lifestyle
29
(Rosen, 1958).
In The Iliad, a poem about the attempts to capture Troy and rescue Helen
from her lover Paris, 140 different wounds are described. The mortality rate
averaged 77.6%, the highest as a result of sword and spear thrusts and the
lowest from superficial arrow wounds. There was considerable need for
nursing care, and Achilles, Patroclus, and other princes often acted as nurses
to the injured. The early stages of Greek medicine reflected the influences of
Egyptian, Babylonian, and Hebrew medicine. Therefore, good medical and
nursing techniques were used to treat these war wounds: The arrow was
drawn or cut out, the wound washed, soothing herbs applied, and the wound
bandaged. However, in sickness in which no wound occurred, an evil spirit
was considered the cause. The Greeks applied rational causes and cures to
external injuries, while internal ailments continued to be linked to spiritual
maladies (Bullough & Bullough, 1978).
Roman Era
During the rise and the fall of the Roman era (31 B.C.–A.D. 476), Greek
culture continued to be a strong influence. The Romans easily adopted Greek
culture and expanded the Greeks’ accomplishments, especially in the fields of
engineering, law, and government. For Romans, the government had an
obligation to protect its citizens, not only from outside aggression such as
warring neighbors, but from inside the civilization, in the form of health
laws. According to Bullough and Bullough (1978), Rome was essentially a
“Greek cultural colony” (p. 20).
Galen of Pergamum (A.D. 129–199), often known as the greatest Greek
physician after Hippocrates, left for Rome after studying medicine in Greece
and Egypt and gained great fame as a medical practitioner, lecturer, and
experimenter. In his lifetime, medicine evolved into a science; he submitted
traditional healing practices to experimentation and was possibly the greatest
medical researcher before the 1600s (Bullough & Bullough, 1978). He was
considered the last of the great physicians of antiquity (Kalisch & Kalisch,
1986).
The Greek physicians and healers certainly made the most contributions
to medicine, but the Romans surpassed the Greeks in promoting the
evolution of nursing. Roman armies developed the notion of a mobile war
nursing unit because their battles took them far from home where they could
be cared for by wives and family. This portable hospital was a series of tents
arranged in corridors; as battles wore on, these tents gave way to buildings
that became permanent convalescent camps at the battle sites (Rosen, 1958).
Many of these early military hospitals have been excavated by archaeologists
along the banks of the Rhine and Danube Rivers. They had wards, recreation
areas, baths, pharmacies, and even rooms for officers who needed a “rest
30
cure” (Bullough & Bullough, 1978). Coexisting were the Greek dispensary
forms of temples, or the iatreia, which started out as a type of physician
waiting room. These eventually developed into a primitive type of hospital,
places for surgical clients to stay until they could be taken home by their
families. Although nurses during the Roman era were usually family
members, servants, or slaves, nursing had strengthened its position in medical
care and emerged during the Roman era as a separate and distinct specialty.
The Romans developed massive aqueducts, bathhouses, and sewer
systems during this era. At the height of the Roman Empire, Rome provided
40 gallons of water per person per day to its 1 million inhabitants, which is
comparable to our rates of consumption today (Rosen, 1958).
31
Middle Ages
Many of the advancements of the Greco-Roman era were reversed during the
Middle Ages (A.D. 476–1453) after the decline of the Roman Empire. The
Middle Ages, or the medieval era, served as a transition between ancient and
modern civilizations. Once again, myth, magic, and religion were
explanations and cures for illness and health problems. The medieval world
was the result of a fusion of three streams of thought, actions, and ways of
life—Greco-Roman, Germanic, and Christian—into one (Donahue, 1985).
Nursing was most influenced by Christianity with the beginning of
deaconesses, or female servants, doing the work of God by ministering to
the needs of others. Deacons in the early Christian churches were apparently
available only to care for men, while deaconesses cared for the needs of
women. The role of deaconesses in the church was considered a forward step
in the development of nursing and in the 1800s would strongly influence the
young Florence Nightingale. During this era, Roman military hospitals were
replaced by civilian ones. In early Christianity, the Diakonia, a kind of
combination outpatient and welfare office, was managed by deacons and
deaconesses and served as the equivalent of a hospital. Jesus served as the
example of charity and compassion for the poor and marginal of society.
Communicable diseases were rampant during the Middle Ages, primarily
because of the walled cities that emerged in response to the paranoia and
isolation of the populations. Infection was next to impossible to control.
Physicians had little to offer, deferring to the church for management of
disease. Nursing roles were carried out primarily by religious orders.
The oldest hospital (other than military hospitals in the Roman era) in
Europe was most likely the Hôtel-Dieu in Lyons, France, founded about 542
by Childebert I, king of France. The Hôtel-Dieu in Paris was founded around
652 by Saint Landry, bishop of Paris. During the Middle Ages, charitable
institutions, hospitals, and medical schools increased in number, with the
religious leaders as caregivers. The word hospital, which is derived from the
Latin word hospitalis, meaning service of guests, was most likely more of a
shelter for travelers and other pilgrims as well as the occasional person who
needed extra care (Kalisch & Kalisch, 1986). Early European hospitals were
more like hospices or homes for the aged, sick pilgrims, or orphans. Nurses
in these early hospitals were religious deaconesses who chose to care for
others in a life of servitude and spiritual sacrifice.
Black Death
During the Middle Ages, a series of horrible epidemics, including the Black
32
Death or bubonic plague, ravaged the civilized world (Diamond, 1997). In
the 1300s, Europe, Asia, and Africa saw nearly half their populations lost to
the bubonic plague. Worldwide, more than 60 million deaths were attributed
to this horrible plague. In some parts of Europe, only one-fourth of the
population survived, with some places having too few survivors alive to bury
the dead. Families abandoned sick children and the sick were often left to die
alone (Cartwright, 1972).
Nurses and physicians were powerless to avert the disease. Black spots
and tumors on the skin appeared, and petechiae and hemorrhages gave the
skin a darkened appearance. There was also acute inflammation of the lungs,
burning sensations, unquenchable thirst, and inflammation of the entire
body. Hardly anyone afflicted survived the third day of the attack. So great
was the fear of contagion that ships carrying bodies of infected persons were
set to sail without a crew to drift from port to port through the North, Black,
and Mediterranean Seas with their dead passengers (Cohen, 1989).
Medieval people knew that this disease was in some way communicable,
but they were unsure of the mode of transmission (Diamond, 1997); hence
the avoidance of victims and a reliance on isolation techniques. During this
time, the practice of quarantine in city ports was developed as a preventive
measure that is still used today (Bullough & Bullough, 1978; Kalisch &
Kalisch, 1986).
33
The Renaissance
During the rebirth of Europe, political, social, and economic advances
occurred along with a tremendous revival of learning. Donahue (1985)
contends that the Renaissance has been “viewed as both a blessing and a
curse” (p. 188). There was a renewed interest in the arts and sciences, which
helped advance medical science (Boorstin, 1985; Bullough & Bullough,
1978). Columbus and other explorers discovered new worlds, and belief in a
sun-centered rather than an Earth-centered universe was promoted by
Copernicus (1473–1543). Sir Isaac Newton’s (1642–1727) theory of gravity
changed the world forever. Gunpowder was introduced, and social and
religious upheavals resulted in the American and French Revolutions at the
end of the 1700s. In the arts and sciences, Leonardo da Vinci, known as one
of “the greatest geniuses of all time,” made a number of anatomic drawings
based on dissection experiences. These drawings have become classics in the
progression of knowledge about the human anatomy. Many artists of this
time left an indelible mark and continue to exert influence today, including
Michelangelo, Raphael, and Titian (Donahue, 1985).
The Reformation
Religious changes during the Renaissance influenced nursing perhaps more
than any other aspect of society. Particularly important was the rise of
Protestantism as a result of the reform movements of Martin Luther (1483–
1546) in Germany and John Calvin (1509–1564) in France and Switzerland.
Although the various sects were numerous in the Protestant movement, the
agreement among the leaders was almost unanimous on the abolition of the
monastic or cloistered career. The effects on nursing were drastic: Monasticaffiliated institutions, including hospitals and schools, were closed, and
orders of nuns, including nurses, were dissolved. Even in countries where
Catholicism flourished, royal leaders seized monasteries frequently.
Religious leaders, such as Martin Luther, who led the Reformation in
1517, were well aware of the lack of adequate nursing care as a result of
these sweeping changes. Luther advocated that each town establish
something akin to a “community chest” to raise funds for hospitals and
nurse visitors for the poor (Dietz & Lehozky, 1963). Thus, the closures of
the monasteries eventually resulted in the creation of public hospitals where
laywomen performed nursing care. It was difficult to find laywomen who
were willing to work in these hospitals to care for the sick, so judges began
giving prostitutes, publically intoxicated women, and poverty-stricken
women the option of going to jail, going to the poorhouse, or working in the
34
public hospital. Unlike the sick wards in monasteries, which were generally
considered to be clean and well managed, the public hospitals were filthy,
disorganized buildings where people went to die while being cared for by
laywomen who were not trained, motivated, or qualified to care for the sick
(Sitzman & Judd, 2014a).
In England, where there had been at least 450 charitable foundations
before the Reformation, only a few survived the reign of Henry VIII, who
closed most of the monastic hospitals (Donahue, 1985). Eventually, Henry
VIII’s son, Edward VI, who reigned from 1547 to 1553, endowed some
hospitals, namely, St. Bartholomew’s Hospital and St. Thomas’ Hospital,
which would eventually house the Nightingale School of Nursing later in the
1800s (Bullough & Bullough, 1978).
35
The Dark Period of Nursing
The last half of the period between 1500 and 1860 is widely regarded as the
“dark period of nursing” because nursing conditions were at their worst
(Donahue, 1985). Education for girls, which had been provided by the nuns
in religious schools, was lost. Because of the elimination of hospitals and
schools, there was no one to pass on knowledge about caring for the sick. As
a result, the hospitals were managed and staffed by municipal authorities;
women entering nursing service often came from illiterate classes, and even
then, there were too few to serve (Dietz & Lehozky, 1963). The lay
attendants who filled the nursing role were illiterate, rough, inconsiderate,
and often immoral and alcoholic. Intelligent women and men could not be
persuaded to accept such a degraded and low-status position in the offensive
municipal hospitals of London. Nursing slipped back into a role of servitude
as menial, low-status work. According to Donahue (1985), when a woman
could no longer make it as a gambler, prostitute, or thief, she might become
a nurse. Eventually, women serving jail sentences for crimes such as
prostitution and stealing were ordered to care for the sick in the hospitals
instead of serving their sentences in the city jail (Dietz & Lehozky, 1963).
The nurses of this era took bribes from clients, became inappropriately
involved with them, and survived the best way they could, often at the
expense of their assigned clients.
Nursing had, during this era, virtually no social standing or organization.
Even Catholic sisters of the religious orders throughout Europe “came to a
complete standstill” professionally because of the intolerance of society
(Donahue, 1985, p. 231). Charles Dickens, in Martin Chuzzlewit (1844),
created the enduring characters of Sairey Gamp and Betsy Prig. Sairey Gamp
was a visiting nurse based on an actual hired attendant whom Dickens had
met in a friend’s home. Sairey Gamp was hired to care for sick family
members but was instead cruel to her clients, stole from them, and ate their
rations; she was an alcoholic and has been immortalized forever as a
reminder of the world in which Florence Nightingale came of age (Donahue,
1985).
In the New World, the first hospital in the Americas, the Hospital de la
Purísima Concepción, was founded some time before 1524 by Hernando
Cortez, the conqueror of Mexico. The first hospital in the continental United
States was erected in Manhattan in 1658 for the care of sick soldiers and
slaves. In 1717, a hospital for infectious diseases was built in Boston; the first
hospital established by a private gift was the Charity Hospital in New
Orleans. A sailor, Jean Louis, donated the endowment for the hospital’s
founding (Bullough & Bullough, 1978).
36
During the 1600s and 1700s, colonial hospitals with little resemblance to
modern hospitals were often used to house the poor and downtrodden.
Hospitals called “pesthouses” were created to care for clients with
contagious diseases; their primary purpose was to protect the public at large,
rather than to treat and care for the clients. Contagious diseases were
rampant during the early years of the American colonies, often being spread
by the large number of immigrants who brought these diseases with them on
their long journey to America. Medicine was not as developed as in Europe,
and nursing remained in the hands of the uneducated. By 1720, average life
expectancy at birth was only around 35 years. Plagues were a constant
nightmare, with outbreaks of smallpox and yellow fever. In 1751, the first
true hospital in the new colonies, Pennsylvania Hospital, was erected in
Philadelphia on the recommendation of Benjamin Franklin (Kalisch &
Kalisch, 1986).
By today’s standards, hospitals in the 1800s were disgraceful, dirty,
unventilated, and contaminated by infections; to be a client in a hospital
actually increased one’s risk of dying. As in England, nursing was considered
an inferior occupation. After the sweeping changes of the Reformation,
educated religious health workers were replaced with lay people who were
“down and outers,” in prison, or had no option left but to work with the
sick (Kalisch & Kalisch, 1986).
37
The Industrial Revolution
During the mid-1700s in England, capitalism emerged as an economic system
based on profit. This emerging system resulted in mass production, as
contrasted with the previous system of individual workers and craftsmen. In
the simplest terms, the Industrial Revolution was the application of machine
power to processes formerly done by hand. Machinery was invented during
this era and ultimately standardized quality; individual craftsmen were forced
to give up their crafts and lands and become factory laborers for the
capitalist owners. All types of industries were affected; this new-found
efficiency produced profit for owners of the means of production. Because of
this, the era of invention flourished, factories grew, and people moved in
record numbers to the work in the cities. Urban areas grew, tenement
housing projects emerged, and overcrowding in cities seriously threatened
individuals’ well-being (Donahue, 1985).
Workers were forced to go to the machines, rather than the other way
around. Such relocations meant giving up not only farming, but a way of life
that had existed for centuries. The emphasis on profit over people led to
child labor, frequent layoffs, and long workdays filled with stressful, tedious,
unfamiliar work. Labor unions did not exist, and neither was there any legal
protection against exploitation of workers, including children (Donahue,
1985). All these rapid changes and often threatening conditions created the
world of Charles Dickens, where, as in his book Oliver Twist, children
worked as adults without question.
According to Donahue (1985), urban life, trade, and industrialization
contributed to these overwhelming health hazards, and the situation was
confounded by the lack of an adequate means of social control. Reforms
were desperately needed, and the social reform movement emerged in
response to the unhealthy by-products of the Industrial Revolution. It was in
this world of the 1800s that reformers such as John Stuart Mill (1806–1873)
emerged. Although the Industrial Revolution began in England, it quickly
spread to the rest of Europe and to the United States (Bullough & Bullough,
1978). The reform movement is critical to understanding the emerging health
concerns that were later addressed by Florence Nightingale. Mill championed
popular education, the emancipation of women, trade unions, and religious
toleration. Other reform issues of the era included the abolition of slavery
and, most important for nursing, more humane care of the sick, the poor,
and the wounded (Bullough & Bullough, 1978). There was a renewed energy
in the religious community with the reemergence of new religious orders in
the Catholic Church that provided service to the sick and disenfranchised.
38
Epidemics had ravaged Europe for centuries, but they became even more
serious with urbanization. Industrialization brought people to cities, where
they worked in close quarters (as compared with the isolation of the farm),
and contributed to the social decay of the second half of the 1800s.
Sanitation was poor or nonexistent, sewage disposal from the growing
population was lacking, cities were filthy, public laws were weak or
nonexistent, and congestion of the cities inevitably brought pests in the form
of rats, lice, and bedbugs, which transmitted many pathogens.
Communicable diseases continued to plague the population, especially those
who lived in these unsanitary environments. For example, during the mid1700s typhus and typhoid fever claimed twice as many lives each year as did
the Battle of Waterloo (Hanlon & Pickett, 1984). Through foreign trade and
immigration, infectious diseases were spread to all of Europe and eventually
to the growing United States.
The Chadwick Report
Edwin Chadwick became a major figure in the development of the field of
public health in Great Britain by drawing attention to the cost of the
unsanitary conditions that shortened the life span of the laboring class and
threatened the wealth of Britain. Although the first sanitation legislation,
which established a National Vaccination Board, was passed in 1837,
Chadwick found in his classic study, Report on an Inquiry into the Sanitary
Conditions of the Labouring Population of Great Britain, that death rates
were high in large industrial cities such as Liverpool. A more startling
finding, from what is often referred to simply as the Chadwick Report, was
that more than half the children of labor-class workers died by age 5,
indicating poor living conditions that affected the health of the most
vulnerable. Laborers lived only half as long as the upper classes.
One consequence of the report was the establishment in 1848 of the first
board of health, the General Board of Health for England (Richardson,
1887). More legislation followed that initiated social reform in the areas of
child welfare, elder care, the sick, the mentally ill, factory health, and
education. Soon sewers and fireplugs, based on an available water supply,
appeared as indicators that the public health linkages from the Chadwick
Report had an impact.
The Shattuck Report
In the United States during the 1800s, waves of epidemics of yellow fever,
smallpox, cholera, typhoid fever, and typhus continued to plague the
population as in England and the rest of the world. As cities continued to
grow in the industrialized young nation, poor workers crowded into larger
cities and suffered from illnesses caused by the unsanitary living conditions
39
(Hanlon & Pickett, 1984). Similar to Chadwick’s classic study in England,
Lemuel Shattuck, a Boston bookseller and publisher who had an interest in
public health, organized the American Statistical Society in 1839 and issued a
census of Boston in 1845. Shattuck’s census revealed high infant mortality
rates and high overall population mortality rates. In 1850, in his Report of
the Massachusetts Sanitary Commission, Shattuck not only outlined his
findings on the unsanitary conditions, but also made recommendations for
public health reform that included the bookkeeping of population statistics
and development of a monitoring system that would provide information to
the public about environmental, food, and drug safety and infectious disease
control (Rosen, 1958). He also called for services for well-child care, schoolage children’s health, immunizations, mental health, health education for all,
and health planning. The Shattuck Report was revolutionary in its scope
and vision for public health, but it was virtually ignored during Shattuck’s
lifetime. Nineteen years later, in 1869, the first state board of health was
formed (Kalisch & Kalisch, 1986).
And Then There Was Nightingale…
Florence Nightingale was named one of the 100 most influential persons of
the last millennium by Life magazine (The 100 people who made the
millennium, 1997). She was one of only eight women identified as such. Of
those eight women, including Joan of Arc, Helen Keller, and Elizabeth I,
Nightingale was identified as a true “angel of mercy,” having reformed
military health care in the Crimean War and used her political savvy to
forever change the way society views the health of the vulnerable, the poor,
and the forgotten. She is probably one of the most written about women in
history (Bullough & Bullough, 1978). Florence Nightingale has become
synonymous with modern nursing.
Florence Nightingale was the second child born on May 12, 1820, to the
wealthy English family of William and Frances Nightingale in her namesake
city, Florence, Italy. As a young child, Florence displayed incredible curiosity
and intellectual abilities not common to female children of the Victorian age.
She mastered the fundamentals of Greek and Latin, and she studied history,
art, mathematics, and philosophy. To her family’s dismay, she believed that
God had called her to be a nurse. Nightingale was keenly aware of the
suffering that industrialization created; she became obsessed with the plight
of the miserable and suffering people. Conditions of general starvation
accompanied the Industrial Revolution, prisons and workhouses overflowed,
and persons in all sections of British life were displaced. She wrote in the
spring of 1842, “My mind is absorbed with the sufferings of man; it besets
me behind and before…. All that the poets sing of the glories of this world
seem to me untrue. All the people that I see are eaten up with care or poverty
40
or disease” (Woodham-Smith, 1951, p. 31).
For Nightingale, her entire life would be haunted by this conflict between
the opulent life of gaiety that she enjoyed and the plight and misery of the
world, which she was unable to alleviate. She was, in essence, an “alien spirit
in the rich and aristocratic social sphere of Victorian England” (Palmer,
1977, p. 14). Nightingale remained unmarried, and at the age of 25, she
expressed a desire to be trained as a nurse in an English hospital. Her parents
emphatically denied her request, and for the next 7 years, she made repeated
attempts to change their minds and allow her to enter nurse training. She
wrote, “I crave for some regular occupation, for something worth doing
instead of frittering my time away on useless trifles” (Woodham-Smith,
1951, p. 162). During this time, she continued her education through the
study of math and science and spent 5 years collecting data about public
health and hospitals (Dietz & Lehozky, 1963). During a tour of Egypt in
1849 with family and friends, Nightingale spent her 30th year in Alexandria
with the Sisters of Charity of St. Vincent de Paul, where her conviction to
study nursing was only reinforced (Tooley, 1910). While in Egypt,
Nightingale studied Egyptian, Platonic, and Hermetic philosophy; Christian
scripture; and the works of poets, mystics, and missionaries in her efforts to
understand the nature of God and her “calling” as it fit into the divine plan
(Calabria, 1996; Dossey, 2000).
The next spring, Nightingale traveled unaccompanied to the Kaiserwerth
Institute in Germany and stayed there for 2 weeks, vowing to return to train
as a nurse. In June 1851, Nightingale took her future into her own hands and
announced to her family that she planned to return to Kaiserwerth and study
nursing. According to Dietz and Lehozky (1963, p. 42), her mother had
“hysterics” and scene followed scene. Her father “retreated into the
shadows,” and her sister, Parthe, expressed that the family name was forever
disgraced (Cook, 1913).
In 1851, at the age of 31, Nightingale was finally permitted to go to
Kaiserwerth, and she studied there for 3 months with Pastor Fliedner. Her
family insisted that she tell no one outside the family of her whereabouts,
and her mother forbade her to write any letters from Kaiserwerth. While
there, Nightingale learned about the care of the sick and the importance of
discipline and commitment of oneself to God (Donahue, 1985). She returned
to England and cared for her then ailing father, from whom she finally
gained some support for her intent to become a nurse—her lifelong dream.
In 1852, Nightingale wrote the essay “Cassandra,” which stands today as
a classic feminist treatise against the idleness of Victorian women. Through
her voluminous journal writings, Nightingale reveals her inner struggle
throughout her adulthood with what was expected of a woman and what she
could accomplish with her life. The life expected of an aristocratic woman in
41
her day was one she grew to loathe; throughout her writings, she poured out
her detestation of the life of an idle woman (Nightingale, 1979, p. 5). In
“Cassandra,” Nightingale put her thoughts to paper, and many scholars
believe that her eventual intent was to extend the essay to a novel. She wrote
in “Cassandra,” “Why have women passion, intellect, moral activity—these
three—in a place in society where no one of the three can be exercised?”
(Nightingale, 1979, p. 37). Although uncertain about the meaning of the
name Cassandra, many scholars believe that it came from the Greek goddess
Cassandra, who was cursed by Apollo and doomed to see and speak the
truth but never to be believed. Nightingale saw the conventional life of
women as a waste of time and abilities. After receiving a generous yearly
endowment from her father, Nightingale moved to London and worked
briefly as the superintendent of the Establishment for Gentlewomen During
Illness hospital, finally realizing her dream of working as a nurse (Cook,
1913).
The Crimean Experience: “I Can Stand Out the
War with Any Man”
Nightingale’s opportunity for greatness came when she was offered the
position of female nursing establishment of the English General Hospitals in
Turkey by the secretary of war, Sir Sidney Herbert. Soon after the outbreak
of the Crimean War, stories of the inadequate care and lack of medical
resources for the soldiers became widely known throughout England
(Woodham-Smith, 1951). The country was appalled at the conditions so
vividly portrayed in the London Times. Pressure increased on Sir Herbert to
react. He knew of one woman who was capable of bringing order out of the
chaos and wrote a letter to Nightingale on October 15, 1854, as a plea for
her service. Nightingale took the challenge from Sir Herbert and set sail with
38 self-proclaimed nurses with varied training and experiences, of whom 24
were Catholic and Anglican nuns. Their journey to the Crimea took a month,
and on November 4, 1854, the brave nurses arrived at Istanbul and were
taken to Scutari the same day. Faced with 3,000 to 4,000 wounded men in a
hospital designed to accommodate 1,700, the nurses went to work (Kalisch
& Kalisch, 1986). The nurses were faced with 4 miles of beds 18 inches
apart. Most soldiers were lying naked with no bedding or blanket. There
were no kitchen or laundry facilities. The little light present took the form of
candles in beer bottles. The hospital was literally floating on an open sewage
lagoon filled with rats and other vermin (Donahue, 1985).
By taking the newly arrived medical equipment and setting up kitchens,
laundries, recreation rooms, reading rooms, and a canteen, Nightingale and
her team of nurses proceeded to clean the barracks of lice and filth.
Nightingale was in her element. She set out not only to provide humane
42
health care for the soldiers but to essentially overhaul the administrative
structure of the military health services (Williams, 1961).
Florence Nightingale and Sanitation
Although Nightingale never accepted the germ theory, she demanded clean
dressings; clean bedding; well-cooked, edible, and appealing food; proper
sanitation; and fresh air. After the other nurses were asleep, Nightingale
made her famous solitary rounds with a lamp or lantern to check on the
soldiers. Nightingale had a lifelong pattern of sleeping few hours, spending
many nights writing, developing elaborate plans, and evaluating implemented
changes. She seldom believed in the “hopeless” soldier, only one who needed
extra attention. Nightingale was convinced that most of the maladies that the
soldiers suffered and died from were preventable (Williams, 1961).
Before Nightingale’s arrival and her radical and well-documented
interventions based on sound public health principles, the mortality rate from
the Crimean War was estimated to be from 42% to 73%. Nightingale is
credited with reducing that rate to 2% within 6 months of her arrival at
Scutari. She did this through careful, scientific epidemiological research
(Dietz & Lehozky, 1963). Upon arriving at Scutari, Nightingale’s first act
was to order 200 scrubbing brushes. The death rate fell dramatically once
Nightingale discovered that the hospital was built literally over an open
sewage lagoon (Andrews, 2003).
According to Palmer (1982), Nightingale possessed the qualities of a good
researcher: insatiable curiosity, command of her subject, familiarity with
methods of inquiry, a good background of statistics, and the ability to
discriminate and abstract. She used these skills to maintain detailed and
copious notes and to codify observations. Nightingale relied on statistics and
attention to detail to back up her conclusions about sanitation, management
of care, and disease causation. Her now-famous “cox combs” are a hallmark
of military health services management by which she diagrammed deaths in
the Army from wounds and from other diseases and compared them with
deaths that occurred in similar populations in England (Palmer, 1977).
Nightingale was first and foremost an administrator: She believed in a
hierarchical administrative structure with ultimate control lodged in one
person to whom all subordinates and offices reported. Within a matter of
weeks of her arrival in the Crimea, Nightingale was the acknowledged
administrator and organizer of a mammoth humanitarian effort. From her
Crimean experience on, Nightingale involved herself primarily in
organizational activities and health planning administration. Palmer contends
that Nightingale “perceived the Crimean venture, which was set up as an
experiment, as a golden opportunity to demonstrate the efficacy of female
nursing” (Palmer, 1982, p. 4). Although Nightingale faced initial resistance
43
from the unconvinced and oppositional medical officers and surgeons, she
boldly defied convention and remained steadfastly focused on her mission to
create a sanitary and highly structured environment for her “children”—the
British soldiers who dedicated their lives to the defense of Great Britain.
Through her resilience and insistence on absolute authority regarding nursing
and the hospital environment, Nightingale was known to send nurses home
to England from the Crimea for suspicious alcohol use and character
weakness.
It was through this success at Scutari that she began a long career of
influence on the public’s health through social activism and reform, health
policy, and the reformation of career nursing. Using her well-publicized
successful “experiment” and supportive evidence from the Crimea,
Nightingale effectively argued the case for the reform and creation of military
health care that would serve as the model for people in uniform to the
present (D’Antonio, 2002). Nightingale’s ideas about proper hospital
architecture and administration influenced a generation of medical doctors
and the entire world, in both military and civilian service. Her work in Notes
on Hospitals, published in 1860, provided the template for the organization
of military health care in the Union Army when the U.S. Civil War erupted in
1861. Her vision for health care of soldiers and the responsibility of the
governments that send them to war continues today; her influence can be
seen throughout the previous century and into this century as health care for
the women and men who serve their country is a vital part of the well-being
of not only the soldiers but for society in general (D’Antonio, 2002).
Returning Home a Heroine: The Political
Reformer
When Nightingale returned to London, she found that her efforts to provide
comfort and health to the British soldier succeeded in making heroes of both
herself and the soldiers (Woodham-Smith, 1951). Both had suffered from
negative stereotypes: The soldier was often portrayed as a drunken oaf with
little ambition or honor, the nurse as a tipsy, self-serving, illiterate,
promiscuous loser. After the Crimean War and the efforts of Nightingale and
her nurses, both returned with honor and dignity, nevermore the
downtrodden and disrespected.
After her return from the Crimea, Florence Nightingale never made a
public appearance, never attended a public function, and never issued a
public statement (Bullough & Bullough, 1978). She single-handedly raised
nursing from, as she put it, “the sink it was” into a respected and noble
profession (Palmer, 1977). As an avid scholar and student of the Greek
writer Plato, Nightingale believed that she had a moral obligation to work
primarily for the good of the community. Because she believed that education
44
formed character, she insisted that nursing must go beyond care for the sick;
the mission of the trained nurse must include social reform to promote the
good. This dual mission of nursing—caregiver and political reformer—has
shaped the profession as we know it today. LeVasseur (1998) contends that
Nightingale’s insistence on nursing’s involvement in a larger political ideal is
the historical foundation of the field and distinguishes us from other
scientific disciplines, such as medicine.
How did Nightingale accomplish this? She effected change through her
wide command of acquaintances: Queen Victoria was a significant admirer
of her intellect and ability to effect change, and Nightingale used her position
as national heroine to get the attention of elected officials in Parliament. She
was tireless and had an amazing capacity for work. She used people. Her
brother-in-law, Sir Harry Verney, was a member of Parliament and often
delivered her “messages” in the form of legislation. When she wanted the
public incited, she turned to the press, writing letters to the London Times
and having others of influence write articles. She was not above threats to
“go public” by certain dates if an elected official refused to establish a
commission or appoint a committee. And when those commissions were
formed, Nightingale was ready with her list of selected people for
appointment (Palmer, 1982).
Nightingale and Military Reforms
The first real test of Nightingale’s military reforms came in the United States
during the Civil War. Nightingale was asked by the Union to advise on the
organization of hospitals and care of the sick and wounded. She sent
recommendations back to the United States based on her experiences and
analysis in the Crimea, and her advisement and influence gained wide
publicity. Following her recommendations, the Union set up a sanitary
commission and provided for regular inspection of camps. She expressed a
desire to help with the Confederate military also but, unfortunately, had no
channel of communication with them (Bullough & Bullough, 1978).
The Nightingale School of Nursing at St. Thomas:
The Birth of Professional Nursing
The British public honored Nightingale by endowing 50,000 pounds sterling
in her name upon her return to England from the Crimea. The money had
been raised from the soldiers under her care and donations from the public.
This Nightingale Fund eventually was used to create the Nightingale School
of Nursing at St. Thomas, which was to be the beginning of professional
nursing (Donahue, 1985). Nightingale, at the age of 40, decided that St.
Thomas’ Hospital was the place for her training school for nurses. While the
negotiations for the school went forward, she spent her time writing Notes
45
on Nursing: What It Is and What It Is Not (Nightingale, 1860). The small
book of 77 pages, written for the British mother, was an instant success. An
expanded library edition was written for nurses and used as the textbook for
the students at St. Thomas. The book has since been translated into many
languages, although it is believed that Nightingale refused all royalties earned
from the publication of the book (Cook, 1913; Tooley, 1910). The nursing
students chosen for the new training school were handpicked; they had to be
of good moral character, sober, and honest. Nightingale believed that the
strong emphasis on morals was critical to gaining respect for the new
“Nightingale nurse,” with no possible ties to the disgraceful association of
past nurses. Nursing students were monitored throughout their 1-year
program both on and off the hospital grounds; their activities were carefully
watched for character weaknesses, and discipline was severe and swift for
violators. Accounts from Nightingale’s journals and notes reveal instant
dismissal of nursing students for such behaviors as “flirtation, using the eyes
unpleasantly, and being in the company of unsavory persons.” Nightingale
contended that “the future of nursing depends on how these young women
behave themselves” (Smith, 1934, p. 234). She knew that the experiment at
St. Thomas to educate nurses and raise nursing to a moral and professional
calling was a drastic departure from the past images of nurses and would
take extraordinary women of high moral character and intelligence.
Nightingale knew every nursing student, or probationer, personally, often
having the students at her house for weekend visits. She devised a system of
daily journal keeping for the probationers; Nightingale herself read the
journals monthly to evaluate their character and work habits. Every nursing
student admitted to St. Thomas had to submit an acceptable “letter of good
character,” and Nightingale herself placed graduate nurses in approved
nursing positions.
One of the most important features of the Nightingale School was its
relative autonomy. Both the school and the hospital nursing service were
organized under the head matron. This was especially significant because it
meant that nursing service began independently of the medical staff in
selecting, retaining, and disciplining students and nurses (Bullough &
Bullough, 1978).
Nightingale was opposed to the use of a standardized government
examination and the movement for licensure of trained nurses. She believed
that schools of nursing would lose control of educational standards with the
advent of national licensure, most notably those related to moral character.
Nightingale led a staunch opposition to the movement by the British Nurses’
Association (BNA) for licensure of trained nurses, one the BNA believed
critical to protecting the public’s safety by ensuring the qualification of
nurses by licensure exam. Nightingale was convinced that qualifying a nurse
by examination tested only the acquisition of technical skills, not the equally
46
important evaluation of character. She believed nursing involved
“divergencies too great for a single standard to be applied” (Nutting &
Dock, 1907; Woodham-Smith, 1951).
Taking Health Care to the Community:
Nightingale and Wellness
Early efforts to distinguish hospital from community health nursing are
evidence of Nightingale’s views on “health nursing,” which she distinguished
from “sick nursing.” She wrote two influential papers, one in 1893, “SickNursing and Health-Nursing” (Nightingale, 1893), which was read in the
United States at the Chicago Exposition, and the second, “Health Teaching
in Towns and Villages” in 1894 (Monteiro, 1985). Both papers praised the
success of prevention-based nursing practice. Winslow (1946) acknowledged
Nightingale’s influence in the United States by being one of the first in the
field of public health to recognize the importance of taking responsibility for
one’s health. She wrote in 1891 that “There are more people to pick us up
and help us stand on our own two feet” (Attewell, 1996). According to
Palmer (1982), Nightingale was a leader in the wellness movement long
before the concept was identified. Nightingale saw the nurse as the key figure
in establishing a healthy society. She saw a logical extension of nursing in
acute hospital settings to the community. Clearly, through her Notes on
Nursing, she visualized the nurse as “the nation’s first bulwark in health
maintenance, the promotion of wellness, and the prevention of disease”
(Palmer, 1982, p. 6).
William Rathbone, a wealthy ship owner and philanthropist, is credited
with the establishment of the first visiting nurse service, which eventually
evolved into district nursing in the community. He was so impressed with the
private duty nursing care that his sick wife had received at home that he set
out to develop a “district nursing service” in Liverpool, England. At his own
expense, in 1859, he developed a corps of nurses trained to care for the sick
poor in their homes (Bullough & Bullough, 1978). He divided the
community into 16 districts; each was assigned a nurse and a social worker
that provided nursing and health education. His experiment in district
nursing was so successful that he was unable to find enough nurses to work
in the districts. Rathbone contacted Nightingale for assistance. Her
recommendation was to train more nurses, and she advised Rathbone to
approach the Royal Liverpool Infirmary with a proposal for opening another
training school for nurses (Rathbone, 1890; Tooley, 1910). The infirmary
agreed to Rathbone’s proposal, and district nursing soon spread throughout
England as successful “health nursing” in the community for the sick poor
through voluntary agencies (Rosen, 1958). Ever the visionary, Nightingale
contended that “Hospitals are but an intermediate stage of civilization. The
47
ultimate aim is to nurse the sick poor in their own homes (1893)” (Attewell,
1996). She also wrote in regard to visiting families at home: “We must not
talk to them or at them but with them (1894)” (Attewell, 1996). A similar
service, health visiting, began in Manchester, England, in 1862 by the
Manchester and Salford Sanitary Association. The purpose of placing “health
visitors” in the home was to provide health information and instruction to
families. Eventually, health visitors evolved to provide preventive health
education and district nurses to care for the sick at home (Bullough &
Bullough, 1978).
Although Nightingale is best known for her reform of hospitals and the
military, she was a great believer in the future of health care, which she
anticipated should be preventive in nature and would more than likely take
place in the home and community. Her accomplishments in the field of
“sanitary nursing” extended beyond the walls of the hospital to include
workhouse reform and community sanitation reform. In 1864, Nightingale
and William Rathbone once again worked together to lead the reform of the
Liverpool Workhouse Infirmary, where more than 1,200 sick paupers were
crowded into unsanitary and unsafe conditions. Under the British Poor Laws,
the most desperately poor of the large cities were gathered into large
workhouses. When sick, they were sent to the Workhouse Infirmary. Trained
nursing care was all but nonexistent. Through legislative pressure and a welldesigned public campaign describing the horrors of the Workhouse
Infirmary, reform of the workhouse system was accomplished by 1867.
Although not as complete as Nightingale had wanted, nurses were in place
and being paid a salary (Seymer, 1954).
The Legacy of Nightingale
Scores have been written about Nightingale—an almost mythic figure in
history. She truly was a beloved legend throughout Great Britain by the time
she left the Crimea in July 1856, 4 months after the war. Longfellow
immortalized this “Lady with the Lamp” in his poem “Santa Filomena”
(Longfellow, 1857). However, when Nightingale returned to London after
the Crimean War, she remained haunted by her experiences related to the
soldiers dying of preventable diseases. She was troubled by nightmares and
had difficulty sleeping in the years that followed (Woodham-Smith, 1983).
Nightingale became a prolific writer and a staunch defender of the causes of
the British soldier, sanitation in England and India, and trained nursing.
As a woman, she was not able to hold an official government post, nor
could she vote. Historians have had varied opinions about the exact nature
of the disability that kept her homebound for the remainder of her life.
Recent scholars have speculated that she experienced post-traumatic stress
disorder (PTSD) from her experiences in the Crimea; there is also
48
considerable evidence that she suffered from the painful disease brucellosis
(Barker, 1989; Young, 1995). She exerted incredible influence through
friends and acquaintances, directing from her sick room sanitation and poor
law reform. Her mission to “cleanse” spread from the military to the British
Empire; her fight for improved sanitation both at home and in India
consumed her energies for the remainder of her life (Vicinus & Nergaard,
1990).
According to Monteiro (1985), two recurrent themes are found
throughout Nightingale’s writings about disease prevention and wellness
outside the hospital. The most persistent theme is that nurses must be trained
differently and instructed specifically in district and instructive nursing. She
consistently wrote that the “health nurse” must be trained in the nature of
poverty and its influence on health, something she referred to as the
“pauperization” of the poor. She also believed that above all, health nurses
must be good teachers about hygiene and helping families learn to better care
for themselves (Nightingale, 1893). She insisted that untrained, “good
intended women” could not substitute for nursing care in the home.
Nightingale pushed for an extensive orientation and additional training,
including prior hospital experience, before one was hired as a district nurse.
She outlined the qualifications in her paper “On Trained Nursing for the Sick
Poor,” in which she called for a month’s “trial” in district nursing, a year’s
training in hospital nursing, and 3 to 6 months training in district nursing
(Monteiro, 1985). She said, “There is no such thing as amateur nursing.”
The second theme that emerged from her writings was the focus on the
role of the nurse. She clearly distinguished the role of the health nurse in
promoting what we today call self-care. In the past, philanthropic visitors in
the form of Christian charity would visit the homes of the poor and offer
them relief (Monteiro, 1985). Nightingale believed that such activities did
little to teach the poor to care for themselves and further “pauperized” them
—dependent and vulnerable—keeping them unhealthy, prone to disease, and
reliant on others to keep them healthy. The nurse then must help the families
at home manage a healthy environment for themselves, and Nightingale saw
a trained nurse as being the only person who could pull off such a feat. She
stated, “Never think that you have done anything effectual in nursing in
London, till you nurse, not only the sick poor in workhouses, but those at
home.”
By 1901, Nightingale lived in a world without sight or sound, leaving her
unable to write. Over the next 5 years, Nightingale lost her ability to
communicate and most days existed in a state of unconsciousness. In
November of 1907, Nightingale was honored with the Order of Merit by
King Edward VII, the first time ever given to a woman. After 50 years, in
May 1910, the Nightingale Training School of Nursing at St. Thomas
celebrated its Jubilee. There were now more than a thousand training schools
49
for nurses in the United States alone (Cook, 1913; Tooley, 1910).
Nightingale died in her sleep around noon on August 13, 1910, and was
buried quietly and without pomp near the family’s home at Embley, her
coffin carried by six sergeants of the British Army. Only a small cross marks
her grave at her request: “FN. Born 1820. Died 1910.” (Brown, 1988). The
family refused a national funeral and burial at Westminster Abbey out of
respect for Nightingale’s last wishes. She had lived for 90 years and 3
months.
Continued Development of
Professional Nursing in the United
Kingdom
Although Florence Nightingale opposed registration, based on the belief that
the essential qualities of a nurse could not be taught, examined, or regulated,
registration in the United Kingdom began in the 1880s. The Hospitals
Association maintained a voluntary registry that was an administrative list.
In an effort to protect the public led by Ethel Fenwick, the BNA was formed
in 1887 with its charter granted in 1893 to unite British nurses and to
provide registration as evidence of systematic training. Finally, in 1919, nurse
registration became law. It took 30 years and the tireless efforts of Ethel
Fenwick, who was supported by other nursing leaders such as Isla Stewart,
Lucy Osbourne, and Mary Cochrane, to achieve mandated registration
(Royal British Nurses’ Association, n.d.).
Another milestone in British nursing history was the founding in 1916 of
the College of Nursing as the professional organization for trained nurses.
For a century, the organization has focused on professional standards for
nurses in their education, practice, and working conditions. Although the
principles of a professional organization and those of a trade union have not
always fit together easily, the Royal College of Nursing has pursued its role
as both the professional organization for nurses and the trade union for
nurses (McGann, Crowther, & Dougall, 2009). Today the Royal College of
Nursing is recognized as the voice of nursing by the government and the
public in the United Kingdom (Royal College of Nursing, n.d.).
The Development of Professional
Nursing in Canada
Marie Lollet Hebert, the wife of a surgeon-apothecary, is credited by many
50
with being the first person in present-day Canada to provide nursing care to
the sick as she assisted her husband after arriving in Quebec in 1617;
however, the first trained nurses arrived in Quebec to care for the sick in
1639. These nurses were Augustine nuns who traveled to Canada to establish
a medical mission to care for the physical and spiritual needs of their
patients, and they established the first hospital in North America, the HôtelDieu de Québec. These nuns also established the first apprenticeship
program for nursing in North America. Jeanne Mance came from France to
the French colony of Montreal in 1642 and founded the Hôtel Dieu de
Montréal in 1645 (Canadian Museum of History, n.d.).
The hospital of the early 19th century did not appeal to the Canadian
public. They were primarily homes for the poor and were staffed by those of
a similar class, rather than by nurses (Mansell, 2004). The decades of the
1830s and 1840s in Canada were characterized by an influx of immigrants
and outbreaks of diseases such as cholera. There is evidence that it was
difficult, especially in times of outbreak, to find sufficient people to care for
the sick. Little is known of the hospital “nurses” of this era, but the
descriptions are unflattering and working in the hospital environment was
difficult. Early midwives did have some standing in the community and were
employed by individuals, although there is record of charitable organizations
also employing midwives (Young, 2010).
During the Crimean War and American Civil War, nurses were extremely
effective in providing treatment and comfort not only to battlefield
casualties, but also to individuals who fell victim to accidents and infectious
disease; however, it was in the North-West Rebellion of 1885 that Canadian
nurses performed military service for the first time. At first, the nursing needs
identified were for duties such as making bandages and preparing supplies. It
soon became apparent that more direct participation by nurses was needed if
the military was to provide effective medical field treatment. Seven nurses,
under the direction of Reverend Mother Hannah Grier Coome, served in
Moose Jaw and Saskatoon, Saskatchewan. Although their tour of duty lasted
only 4 weeks, these women proved that nursing could, and should in the
future, play a vital role in providing treatment to wounded soldiers. In 1899,
the Canadian Army Medical Department was formed, followed by the
creation of the Canadian Army Nursing Service. Nurses received the relative
rank, pay, and allowances of an army lieutenant. Nursing sisters served
thereafter in every military force sent out from Canada, from the South
African War to the Korean War (Veterans Affairs Canada, n.d.).
In 1896, Lady Ishbel Aberdeen, wife of the governor-general of Canada,
visited Vancouver. During this visit, she heard vivid accounts of the hardship
and illness affecting women and children in rural areas. Later that same year
at the National Council of Women, amid similar stories, a resolution was
51
passed asking Lady Aberdeen to found an order of visiting nurses in Canada.
The order was to be a memorial to the 60th anniversary of Queen Victoria’s
ascent to the throne of the British Empire; it received a royal charter in 1897.
The first Victorian Order of Nurses (VON) sites were organized in the cities
of Ottawa, Montreal, Toronto, Halifax, Vancouver, and Kingston. Today
the VON delivers over 75 different programs and services such as prenatal
education, mental health services, palliative care services, and visiting nursing
through 52 local sites staffed by 4,500 healthcare workers and over 9,016
volunteers (VON, 2009).
By the mid to late 19th century, despite previous negativity, nursing came
to be viewed as necessary to progressive medical interventions. To make the
work of the nurse acceptable, changes had to be made to the prevailing view
of nursing. In the 1870s, the ideas of Florence Nightingale were introduced
in Canada. Dr. Theophilus Mack imported nurses who had worked with
Nightingale and founded the first training school for nurses in Canada at St.
Catharine’s General Hospital in 1873. Many hospitals appeared across
Canada from 1890 to 1910, and many of them developed training schools
for nurses. By 1909, there were 70 hospital-based training schools in Canada
(Mansell, 2004).
In 1908, Mary Agnes Snively, along with 16 representatives from
organized nursing bodies, met in Ottawa to form the Canadian National
Association of Trained Nurses (CNATN). By 1924, each of the nine
provinces had a provincial nursing organization with membership in the
CNATN. In 1924, the name of the CNATN was changed to the Canadian
Nurses Association (CNA). CNA is currently a federation of 11 provincial
and territorial nursing associations and colleges representing nearly 150,000
registered nurses (CNA, n.d.).
In 1944, the CNA approved the principle of collective bargaining. In
1946, the Registered Nurses Association of British Columbia became the first
provincial nursing association to be certified as a bargaining agent. By the
1970s, other provincial nursing organizations gained this right. Between
1973 and 1987, nursing unions were created. Today, each of the 10
provinces has a nursing union in addition to a professional association
(Ontario Nurses’ Association, n.d.). One of the best known of these
professional associations is the Registered Nurses’ Association of Ontario
(RNAO). Established in 1925 to advocate for healthy public policy, promote
excellence in nursing practice, increase nursing’s contribution to shaping the
healthcare system, and influence decisions that affect nurses and the public
they serve, the RNAO is the professional association representing registered
nurses, nurse practitioners (NPs), and nursing students in Ontario (RNAO,
n.d.). Through the RNAO, nurses in Canada have led the world in systematic
implementation of evidence-based practice and have made their best practice
52
guidelines available to all nurses to promote safe and effective care of
patients.
As Canadians entered the decade of the 1960s, there was serious concern
about the healthcare system. In 1961, all Canadian provinces signed on to
the Hospital Insurance and Diagnostic Services Act. This legislation created a
national, universal health insurance system. The same year, the Royal
Commission on Health Services was established and presented four
recommendations. One of the recommendations was to examine nursing
education. Prior to this, the CNA had requested a survey of nursing schools
across Canada with the goal of assessing how prepared the schools were for
a national system of accreditation. The findings of this survey, paired with
the commission’s recommendation, led to the establishment of the Canadian
Nurses Foundation (CNF) in 1962. The CNF provides funding for nurses to
further their education and for research related to nursing care (CNF, 2014).
The Canadian Association of Schools of Nursing is the organization that
promotes national nursing education standards and is the national
accrediting agency for university nursing programs in Canada (n.d.).
Nursing in Canada transformed itself to meet the needs of a changing
Canadian society, and in doing so was responsible for a shift from nursing as
a spiritual vocation to a secular but indispensable profession. Nurses’
willingness to respond in times of need, whether economic, epidemic, or war,
contributed to their importance in the healthcare system (Mansell, 2004).
Canadian nursing associations agreed that starting in the year 2000, the basic
educational preparation for the registered nurse would be the baccalaureate
degree, and all provinces and territories launched a campaign known as EP
2000, which later became EP 2005. Currently, the baccalaureate degree
earned from a university is the accepted entry level into nursing practice in
Canada (Mansell, 2004).
The Development of Professional
Nursing in Australia
In the earliest days of the colony, the care of the sick was performed by
untrained convicts. Male attendants undertook the supervision of male
patients and female attendants undertook duties with the female patients.
Attention to hygiene standards was almost nonexistent. In 1885, the poor
health and living conditions of disadvantaged sick persons in Melbourne
prompted a group of concerned citizens to meet and form the Melbourne
District Nursing Society. This society was formed to look after sick poor
persons at home to prevent unnecessary hospitalization. Home visiting
services also have a long history in Australia, with Victoria being the first
state to introduce a district nursing service in 1885, followed by South
53
Australia in 1894, Tasmania in 1896, New South Wales in 1900,
Queensland in 1904, and Western Australia in 1905 (Australian Bureau of
Statistics, 1985).
Australian nurses were involved in military nursing as civilian volunteers
as early as the 1880s (The University of Melbourne, 2015); however,
involvement of Australian women as nurses in war began in 1898 with the
formation of the Australian Nursing Service of New South Wales, which was
composed of 1 superintendent and 24 nurses. Based on the performance of
the nurses, the Australian Army Nursing Service was formed in 1903 under
the control of the federal government. The Royal Australian Army Nursing
Corps (RAANC) had its beginnings in the Australian Army Nursing Service
(RAANC, n.d.). Since that time, Australian nurses have dealt with war, the
sick, the wounded, and the dead. They have served in Australia, in war zones
around the world, in field hospitals, on hospital ships anchored off shore
near battlefields, and on transports (Australian Government, 2009). Other
military opportunities for nurses include the Royal Australian Navy and the
Royal Australian Air Force.
Nursing registration in Australia began in 1920 as a state-based system.
Prior to 1920, nurses received certificates from the hospitals where they
trained, the Australian Trained Nurses Association (ATNA), or the Royal
British Nurses’ Association in order to practice. Today nurses and midwives
are registered through the Nursing and Midwifery Board of Australia
(NMBA), which is made up of member state and territorial boards of nursing
and supported by the Australian Health Practitioner Regulation Agency.
State and territorial boards are responsible for making registration and
notification decisions related to individual nurses or midwives (NMBA, n.d.).
Around the turn of the 20th century, in order to create a formal means of
supporting their role and improve nursing standards and education, the
nurses of South Australia formed the South Australian branch of ATNA. It is
from this organization that the Australian Nursing and Midwifery Federation
in South Australia (ANMFSA) evolved (ANMFSA, 2012). The Australian
Nursing and Midwifery Accreditation Council (ANMAC) is now the
independent accrediting authority for nursing and midwifery under
Australia’s National Registration and Accreditation Scheme. The ANMAC is
responsible for protecting and promoting the safety of the Australian
community by promoting high standards of nursing and midwifery education
through the development of accreditation standards, accreditation of
programs, and assessment of internationally qualified nurses and midwives
for migration (ANMAC, 2014).
In the late 1920s, two nurses, Evelyn Nowland and a Miss Clancy, began
working separately on the idea of a union for nurses and were brought
together by Jessie Street, who saw the improvement of nurses’ wages and
54
conditions as a feminist cause. What is now the New South Wales Nurses
and Midwives’ Association (NSWNMA) was registered as a trade union in
1931 (NSWNMA, 2014). Through the amalgamation of various
organizations, there is now one national organization to represent registered
nurses, enrolled nurses, midwives, and assistants doing nursing work in every
state and territory throughout Australia: the Australian Nursing and
Midwifery Federation (ANMF). The organization was established in 1924
and serves as a union for nurses with an ultimate goal of improving patient
care. The ANMF is now composed of eight branches: the Australian Nursing
and Midwifery Federation (South Australia branch), the NSWNMA, the
Australian Nursing and Midwifery Federation Victorian Branch, the
Queensland Nurses Union, the Australian Nursing and Midwifery Federation
Tasmanian Branch, the Australian Nursing and Midwifery Federation
Australian Capital Territory, the Australian Nursing and Midwifery
Federation Northern Territory, and the Australian Nursing and Midwifery
Federation Western Australian Branch (ANMF, 2015).
Early Nursing Education and
Organization in the United States
Formal nursing education in the United States did not begin until 1862, when
Dr. Marie Zakrzewska opened the New England Hospital for Women and
Children, which had its own nurse training program (Sitzman & Judd,
2014b). Many of the first training schools for nursing were modeled after the
Nightingale School of Nursing at St. Thomas in London. They included the
Bellevue Training School for Nurses in New York City; the Connecticut
Training School for Nurses in New Haven, Connecticut; and the Boston
Training School for Nurses at Massachusetts General Hospital (Christy,
1975; Nutting & Dock, 1907). Based on the Victorian belief in the natural
abilities of women to be sensitive, possess high morals, and be caregivers,
early nursing training required that applicants be female. Sensitivity, high
moral character, purity of character, subservience, and “ladylike” behavior
became the associated traits of a “good nurse,” thus setting the “feminization
of nursing” as the ideal standard for a good nurse. These historical roots of
gender-and race-based caregiving continued to exclude males and minorities
from the nursing profession for many years and still influence career choices
for men and women today. These early training schools provided a stable,
subservient, white female workforce because student nurses served as the
primary nursing staff for these early hospitals. Minority nurses found limited
educational opportunities in this climate. The first African American nursing
school graduate in the United States was Mary P. Mahoney. She graduated
from the New England Hospital for Women and Children in 1879 (Sitzman
& Judd, 2014b).
55
CRITICAL THINKING QUESTIONS✶
Some nurses believe that Florence Nightingale holds nursing back and
represents the negative and backward elements of nursing. This view cites
as evidence that Nightingale supported the subordination of nurses to
physicians, opposed registration of nurses, and did not see mental health
nurses as part of the profession. Wheeler (1999) has gone so far as to say,
“The nursing profession needs to exorcise the myth of Nightingale, not
necessarily because she was a bad person, but because the impact of her
legacy has held the profession back too long.” After reading this chapter,
what do you think? Is Nightingale relevant in the 21st century to the
nursing profession? Why or why not?✶
Nursing education in the newly formed schools was based on accepted
practices that had not been validated by research. During this time in history,
nurses primarily relied on tradition to guide practice, rather than engaging in
research to test interventions; however, scientific advances did help to
improve nursing practice as nurses altered interventions based on knowledge
generated by scientists and physicians. During this time, a nurse, Clara
Maass, gave her life as a volunteer subject in the research of yellow fever
(Sitzman & Judd, 2014b).
A significant report, known simply as the Goldmark Report, Nursing
and Nursing Education in the United States, was released in 1922 and
advocated the establishment of university schools of nursing to train nursing
leaders. The report, initiated by Nutting in 1918, was an exhaustive and
comprehensive investigation into the state of nursing education and training
resulting in a 500-page document. Josephine Goldmark, social worker and
author of the pioneering research of nursing preparation in the United States,
stated,
From our field study of the nurse in public health nursing, in private
duty, and as instructor and supervisor in hospitals, it is clear that
there is need of a basic undergraduate training for all nurses alike,
which should lead to a nursing diploma. (Goldmark, 1923, p. 35)
The first university school of nursing was developed at the University of
Minnesota in 1909. Although the new nurse training school was under the
college of medicine and offered only a 3-year diploma, the Minnesota
program was nevertheless a significant leap forward in nursing education.
Nursing for the Future, or the Brown Report, authored by Esther Lucille
Brown in 1948 and sponsored by the Russell Sage Foundation, was critical of
the quality and structure of nursing schools in the United States. The Brown
Report became the catalyst for the implementation of educational nursing
program accreditation through the National League for Nursing (Brown,
1936, 1948). As a result of the post–World War II nursing shortage, an
56
Associate Degree in Nursing was established by Dr. Mildred Montag in 1952
as a 2-year program for registered nurses (Montag, 1959). In 1950, nursing
became the first profession for which the same licensure exam, the State
Board Test Pool, was used throughout the nation to license registered nurses.
This increased mobility for the registered nurse resulted in a significant
advantage for the relatively new profession of nursing (State board test pool
examination, 1952).
The Evolution of Nursing in the United
States: The First Century of
Professional Nursing
The Profession of Nursing Is Born in the United
States
Early nurse leaders of the 20th century included Isabel Hampton Robb, who
in 1896 founded the Nurses’ Associated Alumnae, which in 1911 officially
became known as the American Nurses Association (ANA); and Lavinia
Lloyd Dock, who became a militant suffragist linking women’s roles as
nurses to the emerging women’s movement in the United States.
Mary Adelaide Nutting, Lavinia L. Dock, Sophia Palmer, and Mary E.
Davis were instrumental in developing the first nursing journal, the
American Journal of Nursing (AJN) in October 1900. Through the ANA
and the AJN, nurses then had a professional organization and a national
journal with which to communicate with each other (Kalisch & Kalisch,
1986).
State licensure of trained nurses began in 1903 with the enactment of
North Carolina’s licensure law for nursing. Shortly thereafter, New Jersey,
New York, and Virginia passed similar licensure laws for nursing. Over the
next several years, professional nursing was well on its way to public
recognition of practice and educational standards as state after state passed
similar legislation.
Margaret Sanger worked as a nurse on the Lower East Side of New
York City in 1912 with immigrant families. She was astonished to find
widespread ignorance among these families about conception, pregnancy,
and childbirth. After a horrifying experience with the death of a woman from
a failed self-induced abortion, Sanger devoted her life to teaching women
about birth control. A staunch activist in the early family planning
movement, Sanger is credited with founding Planned Parenthood of America
57
(Sanger, 1928).
By 1917, the emerging new profession saw two significant events that
propelled the need for additional trained nurses in the United States: World
War I and the influenza epidemic. Nightingale and the devastation of the
Civil War had well established the need for nursing care in wartime. Mary
Adelaide Nutting, now Professor of Nursing and Health at Columbia
University, chaired the newly established Committee on Nursing in response
to the need for nurses as the United States entered the war in Europe. Nurses
in the United States realized early that World War I was unlike previous
wars. It was a global conflict that involved coalitions of nations against
nations and vast amounts of supplies and demanded the organization of all
the nations’ resources for military purposes (Kalisch & Kalisch, 1986). Along
with Lillian Wald and Jane A. Delano, Director of Nursing in the American
Red Cross, Nutting initiated a national publicity campaign to recruit young
women to enter nurses’ training. The Army School of Nursing, headed by
Annie Goodrich as dean, and the Vassar Training Camp for Nurses prepared
nurses for the war as well as home nursing and hygiene nursing through the
Red Cross (Dock & Stewart, 1931). The committee estimated that there were
at the most about 200,000 active “nurses” in the United States, both trained
and untrained, which was inadequate for the military effort abroad (Kalisch
& Kalisch, 1986).
At home, the influenza epidemic of 1917 to 1919 led to increased public
awareness of the need for public health nursing and public education about
hygiene and disease prevention. The successful campaign to attract nursing
students focused heavily on patriotism, which ushered in the new era for
nursing as a profession. By 1918, nursing school enrollments were up by
25%. In 1920, Congress passed a bill that provided nurses with military rank
(Dock & Stewart, 1931). Following close behind, the passage of the
Nineteenth Amendment to the U.S. Constitution granted women the right to
vote.
L…
Essay Writing Service Features
Our Experience
No matter how complex your assignment is, we can find the right professional for your specific task. Achiever Papers is an essay writing company that hires only the smartest minds to help you with your projects. Our expertise allows us to provide students with high-quality academic writing, editing & proofreading services.
Free Features
Free revision policy
$10Free bibliography & reference
$8Free title page
$8Free formatting
$8How Our Dissertation Writing Service Works
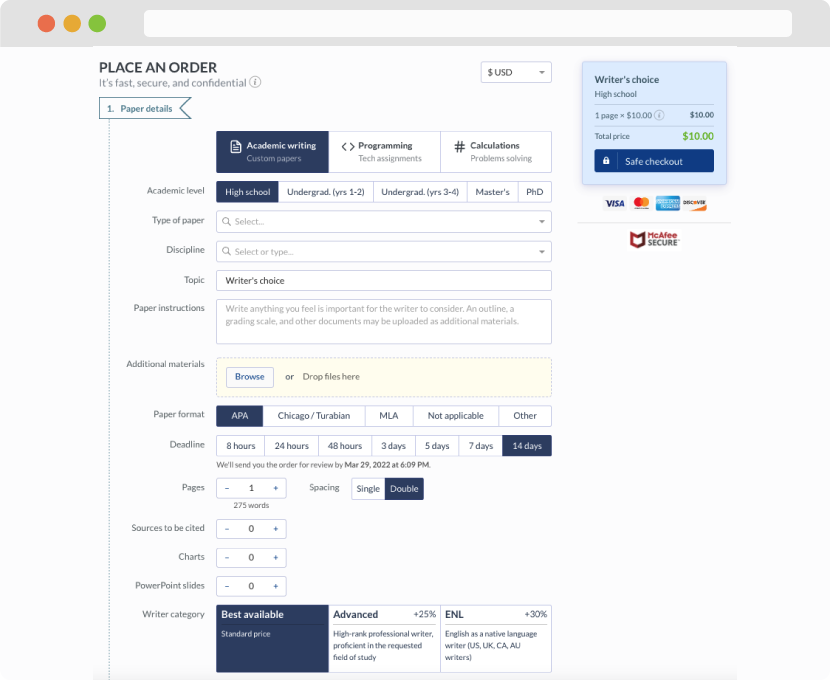
First, you will need to complete an order form. It's not difficult but, if anything is unclear, you may always chat with us so that we can guide you through it. On the order form, you will need to include some basic information concerning your order: subject, topic, number of pages, etc. We also encourage our clients to upload any relevant information or sources that will help.
Complete the order form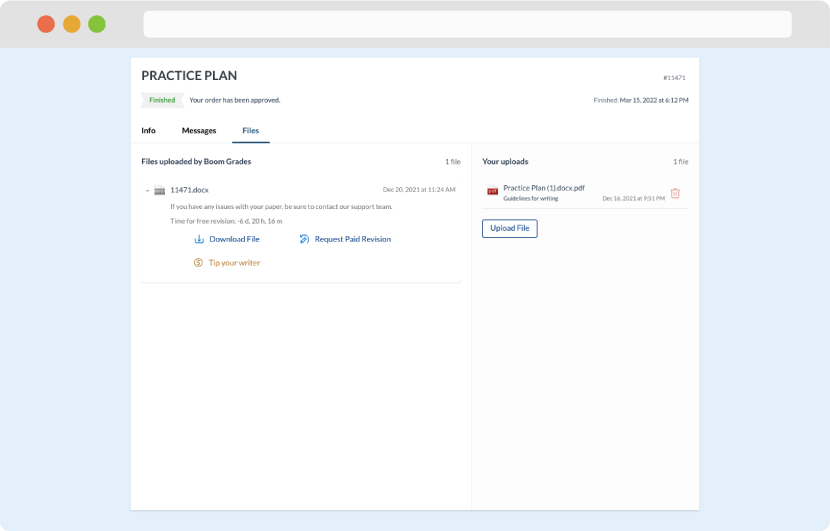
Once we have all the information and instructions that we need, we select the most suitable writer for your assignment. While everything seems to be clear, the writer, who has complete knowledge of the subject, may need clarification from you. It is at that point that you would receive a call or email from us.
Writer’s assignment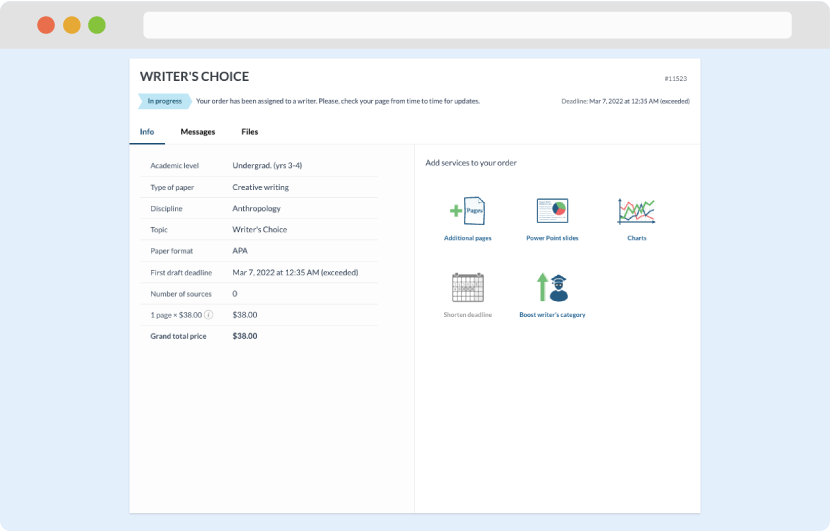
As soon as the writer has finished, it will be delivered both to the website and to your email address so that you will not miss it. If your deadline is close at hand, we will place a call to you to make sure that you receive the paper on time.
Completing the order and download